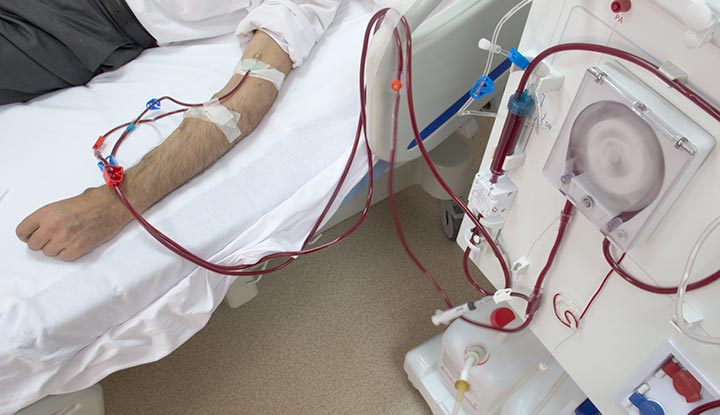
Cardiovascular disease is a main cause of death in dialysis patients. In this disease, a dialysis patient can get a sudden death. Our today’s article is about how do dialysis patients die.
Cardiovascular disease is very common among the dialysis population, and, in addition, it is the most important cause of mortality since it represents 40-50% of the total, much higher than among the general population, especially in younger patients.
The cardiovascular disease begins in the early stages of chronic kidney disease (CKD). When patients start renal replacement therapy already have significant cardiovascular lesions, establishing their prognosis.
The three most important lessons are left ventricular hypertrophy, atherosclerosis, and vascular calcifications. Each has its specific risk factors and their derived clinical consequences, although many factors and clinical manifestations are common. For simplicity, we will describe the three types of injuries separately.
How do dialysis patients die?
Half of the dialysis patients die of cardiovascular disease. When kidney function decreases, the risk of mortality from heart failure increases, to the point that cardiovascular disease is responsible for half of the deaths of people on dialysis, according to data from the Spanish Society of Nephrology (SEN) presented on the occasion of the XX Meeting of its Group for the Prevention of Cardiovascular and Renal Risk (GRUPERVA).
In addition, the presence of cardiovascular risk factors also triples the risk of developing kidney disease. It is estimated that at least 25 percent of patients with cardiovascular disease have relevant chronic kidney disease, although many more would have a silent, undiagnosed involvement.
Kidney disease affects 10 percent of the adult population and more than 20 percent of those over 60, increasing to 40 percent in those affected by diabetes.

At this meeting, organized in Valladolid, attendees have discussed the close connection between kidney and cardiovascular diseases, addressing the latest discoveries, news, and advances.
In this sense, one of the advances addressed during the meeting has been the effect that drugs against diabetes have on cardiovascular problems. Since some are showing that, in addition to reducing sugar levels, they can reduce cardiovascular mortality.
Diagnosis
Cardiac magnetic resonance imaging is the best method for the diagnosis of LVH. However, it is not available in all cases, so echocardiography is the most common method. The left ventricular mass (LVM) is usually calculated using the Devereaux equation with this technique. Based on three parameters determined at the end of diastole:
- End-diastolic diameter (DTD)
- The thickness of the interventricular septum (IVT)
- The thickness of the posterior wall of the left ventricle (PP)
Treatment
The best way to treat LVH is to prevent its development from the early stages of CKD. Once on dialysis, adequate control of arterial hypertension, extracellular volume, anemia, alterations in bone-mineral metabolism, and inflammation are fundamental aspects discussed in other chapters of this work.
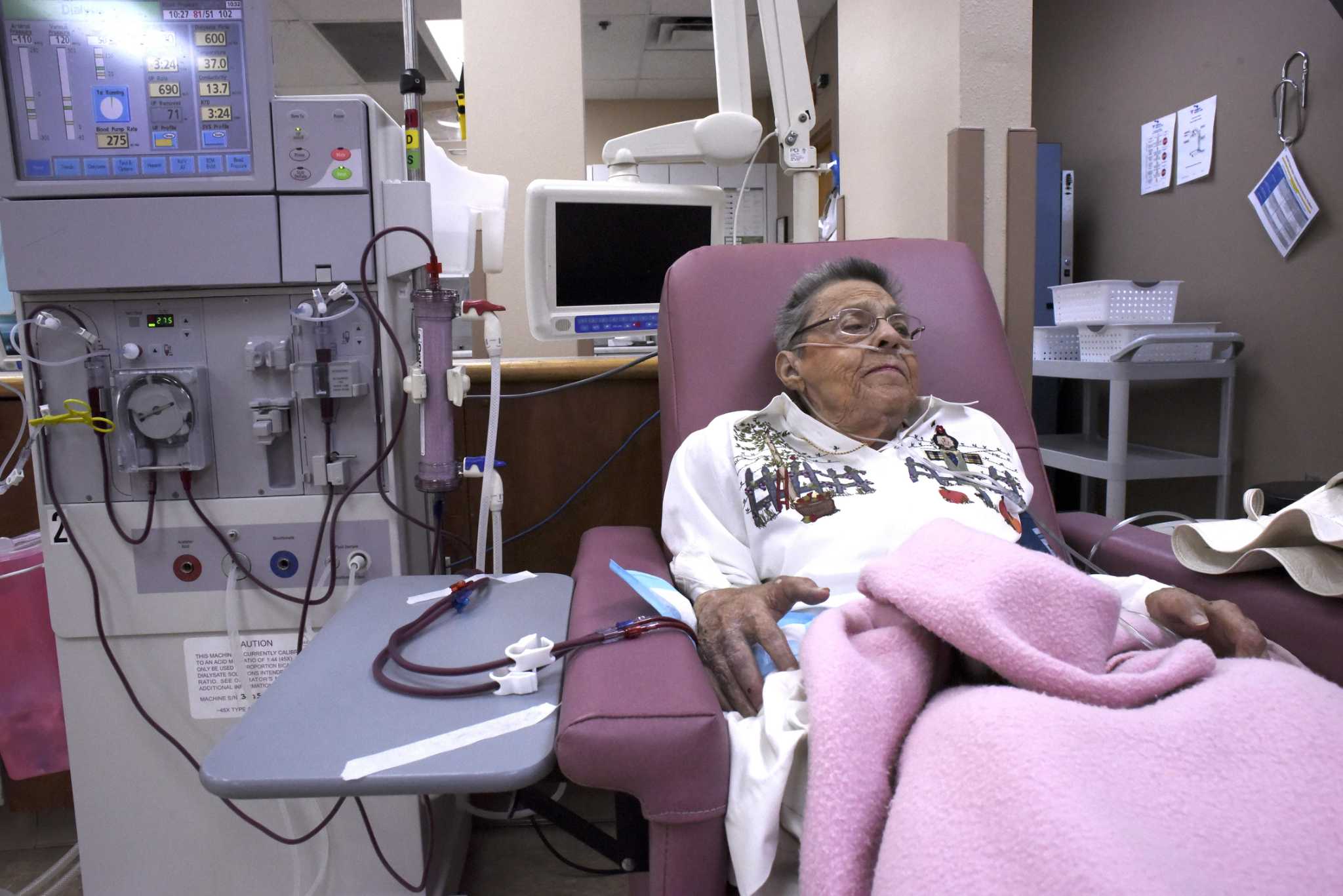
Salt restriction plays a major role in controlling volume overload, hypertension, and LVH. Intakes <5-6 g / day are recommended, although this goal is not easy to achieve in routine practice. In cases where you cannot control hypertension with diet and ultrafiltration, it is preferable to use blockers of the renin-angiotensin system and β-blockers, which may have a beneficial effect on the control LVH and the management of heart failure. Congestive. Daily dialysis or longer dialysis are excellent alternatives in cases of refractory arterial hypertension or frequent episodes of congestive heart failure.
Clinical manifestations
LVH is a mechanism of adaptation of the heart muscle to a sustained excess of work due to pressure or volume overload. In the first case, there is an increase in the thickness of the sarcomeres and a parallel arrangement of the new cells, which leads to an increase in the thickness of the ventricular wall (concentric LVH). The most important causes are high blood pressure, aortic stenosis, and arteriosclerosis. In volume overload, there is a lengthening of the sarcomeres and a series arrangement of the new fibers, which causes an increase in the size of the ventricular cavity (eccentric LVH). The most frequent causes are hydro saline retention and hyperdynamic state of anemia or high output arteriovenous fistulas. However, dialysis treatment is where many predisposing factors for developing left ventricular hypertrophy coincide.
Chronic kidney disease
Another cause of dialysis patients’ dies is dyslipidemia (alteration in blood lipid levels) and its relationship with chronic kidney disease. Dyslipidemia associate with an increase in morbidity and mortality and a greater progression of kidney disease. Since a high level of cholesterol and triglycerides can cause cardiovascular failure, leading to kidney complications. However, rare Kidney patients present with severe dyslipidemia unless other causes of hyperlipidemia are associated.
This international multicenter prospective study (USA and India), implantable cardiac monitors (Reveal XT and Reveal Link) in patients receiving dialysis 3 times a week. It is stable, without a pacemaker or defibrillator, and not a recent infectious episode. You have to give pre- and post-dialysis biological samples weekly and session parameters at each session. Clinically Significant Arrhythmias (ACS) defines as:
- Tachycardia = Ventricular rate ≥ 115BPM for at least 30 seconds.
- Bradycardia = Ventricular rate ≤ 40BPM for at least 6 seconds all arrhythmias confirmed by ECG.
The main objective of this study was to estimate the proportion of patients who presented with SCA at 6 months. The secondary objectives were:
Results
There 66 patients implant with a Reveal monitor. This monitor causes a few complications: 6 delays in healing, one staphylococcus infection, 3 post-insertion pain phenomena, 1 monitor have to remove. 67% of patients (44/66) presented SCA out of 1678. Most of these events were bradycardias (1461 in 13 patients – 20%). Also, 6 patients present with asystole and 5 implants of a pacemaker.
Doctors observe sinus tachycardia, not meeting the criteria for ACS frequently. And finally, they diagnosed only 1 episode of sustained VT. ACS was more frequent during the first dialysis session of the week and in the last 12 hours of the long interval, while AF episodes were more frequent during the dialysis sessions with progressive reduction at a distance. It associates their age and catheter with more frequent SCA. Episodes of bradyarrhythmia were less frequent on days of missed β-blockers and non-dihydropyridine calcium channel blockers. In multivariate analysis, only high sodium pre-dialysis and a calcium dialysis bath associats with more frequent ACS.
In univariate analysis, a cold dialysate (<37 ° C) and a sodium profile were only protective. Episodes of bradyarrhythmias were less frequent on days of missed β-blockers and non-dihydropyridine calcium channel blockers. Multivariate analysis associates only high sodium pre-dialysis and a dialysis bath rich in calcium with more frequent ACS. In univariate analysis, a cold dialysate (<37 ° C) and a sodium profile were only protective.
The cause and consequence of chronic renal failure, you should control hypertension with a low-salt diet and hypotensive therapy. It would also help reduce other cardiovascular risk factors and avoid nephrotoxic drugs or adjust their dosage. Doctors sometimes prescribe certain drugs, which promote erythropoiesis and reduce the absorption of phosphorus. And the elimination of excess water and salt restores the acid-base balance and ensures sufficient intake of vitamin D and calcium.
Adopting a healthy lifestyle also slows down the destruction of the kidneys. Daily physical exercise, stopping smoking, and adopting an adapted diet is essential (reducing animal proteins and intake of phosphorus, sodium, potassium, lipids, and drinking enough).
Functional failures of the kidney
Five stages have been defined in the progression of kidney destruction seen in chronic renal failure. The last, called the terminal stage, corresponds to the moment when both kidneys have lost more than 85% of their function (glomerular filtration rate <15 ml/min).
You may stabilize some patients at stage 5 for several years. But kidney function must most often supplemented by a kidney transplant or by a method of purifying the blood via an extracorporeal bypass (hemodialysis) or peritoneal (peritoneal dialysis). These techniques have revolutionized the management of chronic kidney disease, which was previously fatal.
The hemodialysis filters blood through an artificial membrane for 4 hours, three times a week. It must be accompanied by a prescription of erythropoietin and a suitable diet to overcome metabolic abnormalities not corrected by this treatment, such as anemia and mineral phosphocalcic disorders.
FAQ on How do dialysis patients die
How long could you live a person with dialysis?
Even the cardiovascular causation and the infections are more frequent in all the series. Also, the big races and tenants in the general data can tell the mortality of these things at 14%. 56%.
What is grave hemodialysis?
Since it eliminates the need for hemodialysis, it is even more likely that the recommended treatment in hemodialysis may provoke complications in the form of infusions.
What is hemodialysis, and why not?
In hemodialysis, it is a treatment that the blood’s water filters the toxins, insurance for as they did when the kidneys were healthy. Blood pressure and minerals balance to control the important help in blood insurance, such as potassium, the and sodium-calcium.
Which of the following statements has potential with hemodialysis?
Avoid hitting or cutting your vascular access. Nothing with the heavy arm lift No Be that you have vascular access. However, use it exclusively for hemodialysis. Do not let anyone take your blood pressure or draw blood into your IV arm via one that has vascular access.
Conclusion on How do dialysis patients die
Clinically Significant Arrhythmias are common in dialysis patients and are predominantly episodes of bradycardia/asystole. Five patients had a pacemaker implanted (did this prevent them from sudden death?). These ACS occur more frequently during the first dialysis session of the week and at the end of the long interval between 2 dialyzes. AF, which does not meet the definition of ACS, is more common during dialysis sessions. High sodium pre-dialysis and a calcium-rich bath promote ACS and are easily modifiable factors.